Brain 101 — Part Three
Your Extended Brain — The remarkable network that stretches far beyond your skull
Over the past few weeks, we’ve explored the brain, that wobbly thing that lives in your head: its geography, its cells, its chemical conversations. But here’s something that might surprise you: your nervous system doesn’t stop at your neck.
Today, we’re taking a stroll and venturing beyond the skull to discover the neurons hiding in unexpected places, and why what happens in your gut, your heart, and your body profoundly shapes what happens in your brain.

The So-Called Second Brain: Your Enteric Nervous System
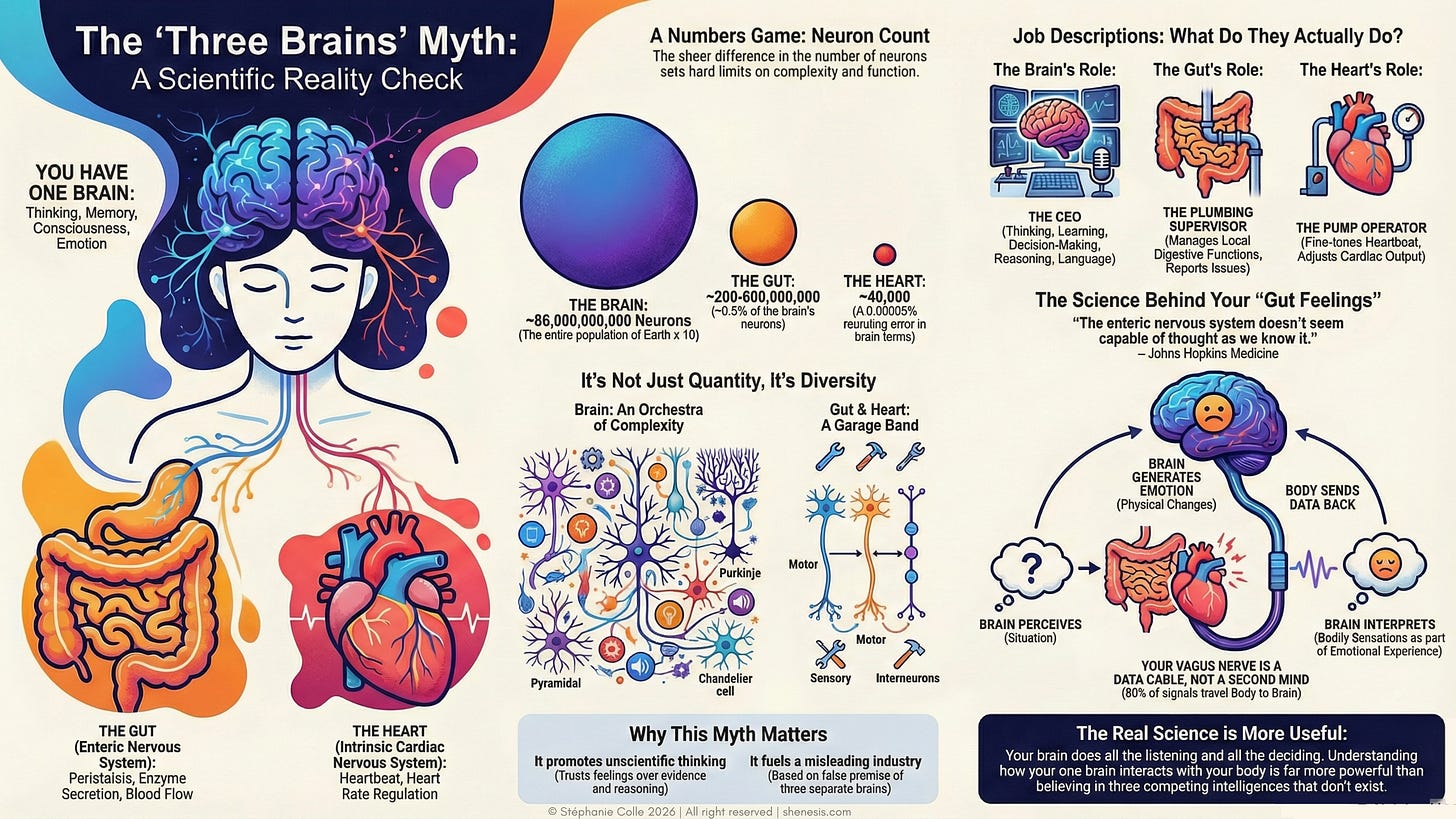
Wrapped around your digestive tract, from oesophagus to rectum, lies a dense network of over 500 million neurons. This is your enteric nervous system (ENS), also often called your “second brain” or “gut brain.”
To put this into perspective, 500 million neurons is more than in your spinal cord, and roughly equivalent to the number in a cat’s brain.
Here’s what makes the ENS remarkable: it can operate independently of your brain. If you severed the connection between your gut and your brain (don’t do this at home), your digestive system would continue to function, capable of sensing food, triggering muscle contractions, managing secretions, coordinating the complex choreography of digestion.
No other organ system can claim this level of autonomy. Your heart needs instructions from the brain to beat (though it has its own rhythm generator). Your lungs need neural signals to breathe. But your gut? It “thinks” for itself.
The Gut-Brain Axis: A Two-Way Street
While the ENS can function independently, it’s in constant communication with your brain. This bidirectional highway, known as the gut-brain axis, is one of the most exciting areas of neuroscience research.
The communication happens through multiple channels:
The vagus nerve: A direct neural connection that carries signals both ways (more on this shortly)
Neurotransmitters: Your gut produces many of the same chemical messengers as your brain
Immune signals: About 70% of your immune system resides in your gut, and immune cells communicate with the brain
The microbiome: The trillions of bacteria in your gut produce compounds that influence brain function
The Serotonin Surprise
Here’s a statistic that often shocks people: roughly 95% of your body’s serotonin is produced in your gut, not your brain.
Serotonin in the gut regulates intestinal movements and secretions. But it also sends signals to the brain via the vagus nerve, influencing mood, appetite, and sleep. This is why gut issues often come with psychological symptoms and vice versa.
“Trust your gut” isn’t just a saying. It’s neuroscience.
The Vagus Nerve: Your Body’s Information Superhighway
The vagus nerve (from the Latin for “wanderer”) is the longest cranial nerve in your body, running from your brainstem through your neck, heart, and lungs, all the way down to your abdomen. It’s the primary channel of the gut-brain axis.
Here’s the key insight: about 80% of the vagus nerve’s fibres are sensory, carrying information from the body to the brain. Only 20% carry commands from the brain to the body. Your brain is listening to your body far more than it’s directing it.
The vagus nerve is also central to your parasympathetic nervous system, the “rest and digest” mode that counterbalances “fight or flight.” A well-functioning vagus nerve (high “vagal tone”) is associated with:
Better emotional regulation
Lower inflammation
Healthier heart rate variability
Better digestion
Improved stress resilience
Boosting Your Vagal Tone
The good news: vagal tone isn’t fixed. You can strengthen it through:
Slow, deep breathing: Especially with a longer exhale than inhale (try 4 counts in, 6-8 counts out)
Cold exposure: Cold water on your face, cold showers (the vagus nerve responds to cold)
Singing, humming, or gargling: These activate the vagus nerve through throat muscles
Meditation and yoga: Particularly practices that focus on breath
Social connection and laughter: Positive social interaction stimulates vagal activity
The Microbiome: Your Bacterial Brain Trust
Living alongside your enteric neurons are trillions of bacteria, fungi (shrooms!), and other microorganisms, collectively called your gut microbiome. The relationship between these microbes and your brain is so significant that some researchers call it the “microbiome-gut-brain axis.”
Your gut bacteria:
Produce neurotransmitters (including serotonin, GABA, and dopamine)
Generate short-chain fatty acids that influence brain function
Modulate inflammation throughout the body, including the brain
Influence the blood-brain barrier’s integrity
Communicate directly with the vagus nerve
Research increasingly links gut microbiome composition to anxiety, depression, cognitive function, and even neurodegenerative diseases. The field is young, but the implications are profound: caring for your gut bacteria may be a form of caring for your brain.
The Heart’s Little Brain
Your gut isn’t the only organ with its own neural network. Your heart contains approximately 40,000 neurons, enough to be called the “heart brain” or “intrinsic cardiac nervous system.”
These cardiac neurons don’t just relay signals from the brain, they can process information and make decisions locally. They’re involved in regulating heart rhythm, sensing hormones and chemicals in the blood, and sending information back to the brain about the body’s emotional and physical state.
This is why emotional states affect heart rhythm and why heart rhythm affects emotional states. It’s a bidirectional relationship. Practices that create coherent heart rhythm patterns (like slow breathing, gratitude, or meditation) send calming signals to the brain.
The Whole-Body Brain
Beyond the gut and heart, neurons are distributed throughout your body:
Skin neurons: Your skin contains sensory neurons that detect touch, temperature, and pain. Emerging research suggests they may do more processing than we thought.
Peripheral nervous system: Sensory and motor neurons throughout your body carry information to and from your central nervous system.
Autonomic nervous system: Controls unconscious functions like breathing, digestion, and heart rate through neurons distributed throughout your organs.
Your brain isn’t just in your head, it’s a distributed network spread throughout your entire body.
What This Means for Brain Health
Understanding the extended brain and the science behind it changes how we think about brain health:
Gut health IS brain health: The foods you eat, the diversity of your microbiome, and the integrity of your gut lining directly influence brain function.
Body-based practices matter: Yoga, breathwork, cold exposure, and other somatic practices aren’t just “wellness trends” — they’re ways of directly influencing your neural network.
Emotions are embodied: That “gut feeling” or “heartache” isn’t metaphorical — your emotions are processed throughout your body, not just in your head.
Inflammation anywhere is inflammation everywhere: Chronic gut inflammation, for example, can trigger brain inflammation via the gut-brain axis.
All Together Now
Over these three weeks, we’ve journeyed from the macro to the micro and back out again:
Part 1: We mapped the brain’s geography: lobes, structures, regions
Part 2: We zoomed into neurons, synapses, and the chemical conversations that create thought
Part 3: We zoomed out to see the brain as an extended network spread throughout the body
The picture that emerges is both humbling and empowering. Humbling, because the complexity is staggering and we’ve barely scratched the surface of what neuroscience is discovering. Empowering, because the brain is not a fixed, fragile organ at the mercy of genetics and time. It’s a dynamic, responsive, plastic system that reshapes itself based on how we live.
Every choice you make, from what you eat, how you move, how well you sleep, to how you manage stress, whether you keep learning, how you nurture your relationships, is a vote for the brain you’ll have tomorrow.
This is the foundation of everything I do in The Brain Reset: understanding the brain so we can support it.
Next week, we return to our regular programming but now with a shared vocabulary. When I mention the hippocampus, you’ll know what I mean. When I talk about the gut-brain axis, you’ll understand why it matters. When I recommend specific foods or practices, you’ll see how they connect to actual neural structures and processes.
Knowledge is power. And you now have more power over your brain health than you did three weeks ago.
Brain 101 — Part One
I realised something recently and it’s slightly embarrassing: I’ve been writing a brain health newsletter for almost a year now, and I’ve never properly introduced you to the brain, the star of this show.
Brain 101 — Part Two
Two weeks ago, we took a tour of your brain’s geography: the lobes, the limbic system, the major structures. But knowing where things happen is only half the story.
🧠 Your Brain Reset Experience
Free
All public posts on brain health, cognitive resilience, and pro-ageing midlife culture, dropped once a week, on Wednesday
Paid
Full access to the complete archive
Exclusive deep dives into stress regulation, memory, focus, and nervous system health
Quarterly Brain Health Workbooks with practical exercises, audits, and implementation tools
→ If this sparked something in you, give this post a like.
→ If you have a thought to share or just want to chime in, leave a comment.
→ And if it made you rethink something and you want to spread the word, restack.
The Brain Reset is more than a newsletter. It’s a conversation about ageing on our own terms. Every interaction helps it grow. Let’s rethink midlife. Redefine ageing. And rewrite what comes next.





If the gut has more neurons than the spinal cord, "gut feelings" are literally a second opinion from a cat-sized brain. It makes you realize that physical health is the literal foundation of clear thinking!
This is a beautiful “systems neuroscience” primer, and I love that you’re teaching people the most important upgrade: the brain isn’t a standalone organ, it’s a distributed network in constant conversation with the body. 
A few physician-scientist notes that I think strengthen (and slightly refine) your message:
1. The enteric nervous system point lands: it’s remarkably autonomous and richly innervated, which helps explain why gut function so reliably shapes mood, sleep, and cognition. 
2. Small nuance on the serotonin line that often gets oversimplified: yes, the majority of serotonin is produced peripherally (largely in the gut), but most peripheral serotonin doesn’t cross the blood–brain barrier. The brain’s serotonin is synthesized locally. The “link” is still real, just via vagal/immune/metabolic signaling rather than serotonin itself traveling from gut → brain. 
3. Your vagus nerve framing is excellent, and the “80% afferent” stat is the key insight that changes how people think about stress regulation: the brain is continuously reading the body. 
4. I also appreciate the way you validate “body-based” practices without drifting into mysticism. Breathwork, cold face immersion, humming/singing; these are low-tech tools that can plausibly shift autonomic balance and perceived threat, which then cascades into sleep and inflammation. 
The larger takeaway is the one you end on: brain health is not a one-pill problem. It’s circadian integrity, gut ecology, autonomic tone, movement, and social safety working together over time. This series is doing exactly what good science communication should: giving people a map and a sense of agency.